There are about 20,000 new cases of thyroid cancer each year in the United States. Females are more likely to have thyroid cancer at a ratio of three to one. Thyroid cancer can occur in any age group, although it is most common after age 30 and its aggressiveness increases significantly in older patients. The majority of patients present with a nodule on their thyroid which typically does not cause symptoms. Remember, over 99% of thyroid nodules are not cancer! But, when a thyroid cancer does begin to grow within a thyroid gland, it almost always does so within a discrete nodule within the thyroid.
Cold nodule in thyroid
Occasionally, symptoms such as hoarseness, neck pain, and enlarged lymph nodes do occur. Although as much as 75 % of the population will have thyroid nodules, the vast majority are benign. Young people usually don't have thyroid nodules, but as we get older, more and more of us will develop a nodule. By the time we are 80, 90% of us will have at least one nodule.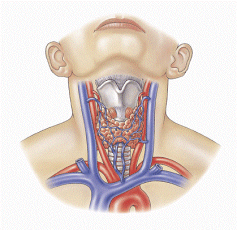 Far less than 1% of all thyroid nodules are malignant. A nodule which is cold on scan (shown in photo outlined in red and yellow) is more likely to be malignant, nevertheless, the majority of these are benign as well. A lot of information about thyroid nodules and the potential of these nodules to be malignant is contained on 3 pages about nodules:
Far less than 1% of all thyroid nodules are malignant. A nodule which is cold on scan (shown in photo outlined in red and yellow) is more likely to be malignant, nevertheless, the majority of these are benign as well. A lot of information about thyroid nodules and the potential of these nodules to be malignant is contained on 3 pages about nodules:
1. Introduction to thyroid nodules
2. The workup of thyroid nodules and the role of Fine Needle Aspiration Biopsy (FNA)
3. The role of thyroid ultrasound and what it means
Types of Thyroid Cancer
There are four types of thyroid cancer some of which are much more common than others.
* Papillary and/or mixed papillary/follicular ~ 78%
* Follicular and/or Hurthle cell ~ 17%
* Medullary ~ 4%
* Anaplastic ~ 1%
Note, Chief Justice William Rehnquist had anaplastic thyroid cancer. After reading this overview page on thyroid cancer, click here to read more about Chief Justice William Rehnquist and his classic battle with the worst kind of thyroid cancer.
What's the Prognosis ?
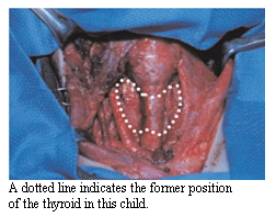
Most thyroid cancers are very curable. In fact, the most common types of thyroid cancer (papillary and follicular) are the most curable. In younger patients, both papillary and follicular cancers can be expected to have better than 97% cure rate if treated appropriately. Both papillary and follicular cancers are typically treated with complete removal of the lobe of the thyroid which harbors the cancer, PLUS, removal of most or all of the other side. The bottom line, most thyroid cancers are papillary thyroid cancer, and this is one of the most curable cancers of ALL cancers that humans get. As we often tell our patients, if you must choose a type of cancer to have, papillary cancer would be your choice. Treat it correctly and the cure rate is extremely high!
Medullary cancer of the thyroid is significantly less common, but has a worse prognosis. Medullary cancers tend to spread to large numbers of lymph nodes very early on, and therefore requires a much more aggressive operation than does the more localized cancers such as papillary and follicular. This cancer requires complete thyroid removal PLUS a dissection to remove the lymph nodes of the front and sides of the neck.
The least common type of thyroid cancer is anaplastic which has a very poor prognosis. Anaplastic thyroid cancer tends to be found after it has spread and is not cured in most cases (it is very uncommon to survive anaplastic thyroid cancer). Often an operation cannot remove all the tumor. These patients often require a tracheostomy during the treatment, and treatment is much more aggressive than for other types of thyroid cancer--because this cancer is much more aggressive.
Chemotherapy
Thyroid cancer is unique among cancers, in fact, thyroid cells are unique among all cells of the human body. They are the only cells which have the ability to absorb Iodine. Iodine is required for thyroid cells to produce thyroid hormone, so they absorb it out of the bloodstream and concentrate it inside the cell. Most thyroid cancer cells retain this ability to absorb and concentrate iodine. This provides a perfect "chemotherapy" strategy. Radioactive Iodine is given to the patient with thyroid cancer after their cancer has been removed. If there are any normal thyroid cells or thyroid cancer cells remain in the patient's body (and any thyroid cancer cells retaining this ability to absorb iodine) then these cells will absorb and concentrate the radioactive "poisonous" iodine.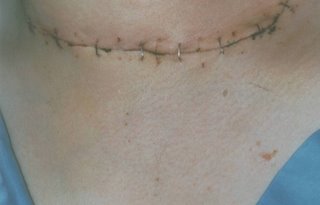 Since all other cells of our bodies cannot absorb the toxic iodine, they are unharmed. The thyroid cancer cells, however, will concentrate the poison within themselves and the radioactivity destroys the cell from within. No sickness. No hair loss. No nausea. No diarrhea. No pain. More about the use of radioactive iodine on the pages for each specific thyroid cancer type.
Since all other cells of our bodies cannot absorb the toxic iodine, they are unharmed. The thyroid cancer cells, however, will concentrate the poison within themselves and the radioactivity destroys the cell from within. No sickness. No hair loss. No nausea. No diarrhea. No pain. More about the use of radioactive iodine on the pages for each specific thyroid cancer type.
Most, but not all patients with thyroid cancer need radioactive iodine treatments after their surgery. This is important to know. Almost all, however, should have the iodine treatment if a cure is to be expected. Just who needs it and who doesn't is a bit more detailed than can be outlined here. Patients with medullary cancer of they thyroid usually do not need iodine therapy...because medullary cancers almost never absorb the radioactive iodine. Some small papillary cancers treated with a total thyroidectomy may not need iodine therapy as well, but for a different reason. These cancers are often cured with simple (complete) surgical therapy alone. Important!!! This varies from patient to patient and from cancer to cancer. Don't look for easy answers here. This decision will be made between the surgeon, the patient, and the referring endocrinologist or internist. Remember, radioactive iodine therapy is extremely safe. If you need it, take it. And, as we often tell our patients, radioactive iodine has a near zero complication rate, so if there is a chance that it will help... take it!
Source - http://www.endocrineweb.com/thyroidca.html
Cold nodule in thyroid
Occasionally, symptoms such as hoarseness, neck pain, and enlarged lymph nodes do occur. Although as much as 75 % of the population will have thyroid nodules, the vast majority are benign. Young people usually don't have thyroid nodules, but as we get older, more and more of us will develop a nodule. By the time we are 80, 90% of us will have at least one nodule.
 Far less than 1% of all thyroid nodules are malignant. A nodule which is cold on scan (shown in photo outlined in red and yellow) is more likely to be malignant, nevertheless, the majority of these are benign as well. A lot of information about thyroid nodules and the potential of these nodules to be malignant is contained on 3 pages about nodules:
Far less than 1% of all thyroid nodules are malignant. A nodule which is cold on scan (shown in photo outlined in red and yellow) is more likely to be malignant, nevertheless, the majority of these are benign as well. A lot of information about thyroid nodules and the potential of these nodules to be malignant is contained on 3 pages about nodules:1. Introduction to thyroid nodules
2. The workup of thyroid nodules and the role of Fine Needle Aspiration Biopsy (FNA)
3. The role of thyroid ultrasound and what it means
Types of Thyroid Cancer
There are four types of thyroid cancer some of which are much more common than others.
* Papillary and/or mixed papillary/follicular ~ 78%
* Follicular and/or Hurthle cell ~ 17%
* Medullary ~ 4%
* Anaplastic ~ 1%
Note, Chief Justice William Rehnquist had anaplastic thyroid cancer. After reading this overview page on thyroid cancer, click here to read more about Chief Justice William Rehnquist and his classic battle with the worst kind of thyroid cancer.
What's the Prognosis ?

Most thyroid cancers are very curable. In fact, the most common types of thyroid cancer (papillary and follicular) are the most curable. In younger patients, both papillary and follicular cancers can be expected to have better than 97% cure rate if treated appropriately. Both papillary and follicular cancers are typically treated with complete removal of the lobe of the thyroid which harbors the cancer, PLUS, removal of most or all of the other side. The bottom line, most thyroid cancers are papillary thyroid cancer, and this is one of the most curable cancers of ALL cancers that humans get. As we often tell our patients, if you must choose a type of cancer to have, papillary cancer would be your choice. Treat it correctly and the cure rate is extremely high!
Medullary cancer of the thyroid is significantly less common, but has a worse prognosis. Medullary cancers tend to spread to large numbers of lymph nodes very early on, and therefore requires a much more aggressive operation than does the more localized cancers such as papillary and follicular. This cancer requires complete thyroid removal PLUS a dissection to remove the lymph nodes of the front and sides of the neck.
The least common type of thyroid cancer is anaplastic which has a very poor prognosis. Anaplastic thyroid cancer tends to be found after it has spread and is not cured in most cases (it is very uncommon to survive anaplastic thyroid cancer). Often an operation cannot remove all the tumor. These patients often require a tracheostomy during the treatment, and treatment is much more aggressive than for other types of thyroid cancer--because this cancer is much more aggressive.
Chemotherapy
Thyroid cancer is unique among cancers, in fact, thyroid cells are unique among all cells of the human body. They are the only cells which have the ability to absorb Iodine. Iodine is required for thyroid cells to produce thyroid hormone, so they absorb it out of the bloodstream and concentrate it inside the cell. Most thyroid cancer cells retain this ability to absorb and concentrate iodine. This provides a perfect "chemotherapy" strategy. Radioactive Iodine is given to the patient with thyroid cancer after their cancer has been removed. If there are any normal thyroid cells or thyroid cancer cells remain in the patient's body (and any thyroid cancer cells retaining this ability to absorb iodine) then these cells will absorb and concentrate the radioactive "poisonous" iodine.
 Since all other cells of our bodies cannot absorb the toxic iodine, they are unharmed. The thyroid cancer cells, however, will concentrate the poison within themselves and the radioactivity destroys the cell from within. No sickness. No hair loss. No nausea. No diarrhea. No pain. More about the use of radioactive iodine on the pages for each specific thyroid cancer type.
Since all other cells of our bodies cannot absorb the toxic iodine, they are unharmed. The thyroid cancer cells, however, will concentrate the poison within themselves and the radioactivity destroys the cell from within. No sickness. No hair loss. No nausea. No diarrhea. No pain. More about the use of radioactive iodine on the pages for each specific thyroid cancer type.Most, but not all patients with thyroid cancer need radioactive iodine treatments after their surgery. This is important to know. Almost all, however, should have the iodine treatment if a cure is to be expected. Just who needs it and who doesn't is a bit more detailed than can be outlined here. Patients with medullary cancer of they thyroid usually do not need iodine therapy...because medullary cancers almost never absorb the radioactive iodine. Some small papillary cancers treated with a total thyroidectomy may not need iodine therapy as well, but for a different reason. These cancers are often cured with simple (complete) surgical therapy alone. Important!!! This varies from patient to patient and from cancer to cancer. Don't look for easy answers here. This decision will be made between the surgeon, the patient, and the referring endocrinologist or internist. Remember, radioactive iodine therapy is extremely safe. If you need it, take it. And, as we often tell our patients, radioactive iodine has a near zero complication rate, so if there is a chance that it will help... take it!

Source - http://www.endocrineweb.com/thyroidca.html
*Let share what ladybugsandbees said about thyroid..(thanks lady)


